Logic of medical language Abstract
Logic of medical language
Abstract
Medical practice is built on language: symptoms are told, histories are narrated, and diagnoses are written. Yet medical language is not a fully formal system—despite its technical vocabulary, it remains an extension of natural language, and therefore inherits its structural vulnerabilities: ambiguity, vagueness, context-dependence, and semantic drift across specialties. This chapter examines how these limits are not minor “communication issues” but a genuine diagnostic risk, capable of producing divergent interpretations and, in some cases, serious clinical error.
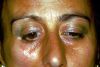
Through an emblematic clinical narrative (the “Mary Poppins” case, a fictional name used for clarity), the chapter shows how the same patient report—e.g., “right-sided orofacial pain,” “jaw locking,” “skin changes,” “muscle contractions”—can generate different diagnostic trajectories depending on the interpretive key applied by each clinician. The dentist may frame the problem within temporomandibular disorders (TMD), occlusion, muscles, and joint imaging; the neurologist may privilege neuropathic mechanisms, central-peripheral integration, and neurophysiological constructs. The patient’s own language, shaped by lived experience and incomplete semantics, adds another layer of distortion. The result is not simply disagreement, but an epistemic gap: the biological “message” exists, yet the words used to express it do not reliably preserve its meaning.
To make this mechanism intuitive, the chapter proposes the metaphor of an encrypted code: the biological system transmits information through signals, patterns, and dynamics that are not directly readable in everyday language. In this view, words become a lossy translation of a deeper “machine-language” level. The crucial question becomes: which interpretive logic is being applied when decoding clinical information—classical, probabilistic, fuzzy, or systems logic? Different “keys” can produce different outputs from the same underlying reality.
This perspective supports a broader shift in diagnostic thinking. Instead of treating symptoms as final objects, the clinician is invited to treat them as encoded outputs of a complex system evolving in time. Measurement and formal reasoning are therefore not decorative: they are instruments for reducing semantic noise and increasing observability of the system’s internal state. Ultimately, Masticationpedia frames the problem as paradigmatic: improving diagnosis requires not only better technology, but a more rigorous logic of meaning—capable of integrating context, temporal dynamics, and interdisciplinary semantics.
🧠 Three guiding questions (with essential answers)
1️⃣ What: why is medical language structurally fragile, even when it uses technical terms? Because it remains an extension of natural language: its words are context-dependent and can be ambiguous or vague. The same term (e.g., “orofacial pain”) may carry different meanings for patient, dentist, and neurologist.
2️⃣ Why: how can semantic ambiguity produce real diagnostic errors? Because clinicians decode the same narrative through different “keys” (disciplinary contexts). Without shared semantics, the clinical message can be distorted, leading to divergent differential diagnoses and inconsistent therapeutic strategies.
3️⃣ How: what is the proposed solution in this chapter? Shift from symptom-as-word to symptom-as-encoded output of a complex system. Use clearer logical frameworks (classical/probabilistic/fuzzy/systems) and measurable signals to improve “observability” and reduce semantic noise in diagnosis.
🔒 Access to the full chapter
👤 Approved users — click on your profile icon and return to the Book Index to read the complete chapter.
🔑 New readers — sign in via LinkedIn to request access.
- Stanley DE, Campos DG, «The logic of medical diagnosis», in Perspect Biol Med, 2013».
PMID:23974509
DOI:10.1353/pbm.2013.0019
- Croskerry P, «Adaptive expertise in medical decision making», in Med Teach, 2018».
PMID:30033794
DOI:10.1080/0142159X.2018.1484898
- Townsend GC, Brook AH, «The face, the future, and dental practice: how research in craniofacial biology will influence patient care», in Aust Dent J, Australian Dental Association, 2014».
PMID:24646132
DOI:10.1111/adj.12157
- Sperber GH, Sperber SM, «The genesis of craniofacial biology as a health science discipline», in Aust Dent J, Australian Dental Association, 2014».
PMID:24495071
DOI:10.1111/adj.12131
- Brook AH, Brook O'Donnell M, Hone A, Hart E, Hughes TE, Smith RN, Townsend GC, «General and craniofacial development are complex adaptive processes influenced by diversity», in Aust Dent J, Australian Dental Association, 2014».
PMID:24617813
DOI:10.1111/adj.12158
- Williams SD, Hughes TE, Adler CJ, Brook AH, Townsend GC, «Epigenetics: a new frontier in dentistry», in Aust Dent J, Australian Dental Association, 2014».
PMID:24611746
DOI:10.1111/adj.12155
- Yong R, Ranjitkar S, Townsend GC, Brook AH, Smith RN, Evans AR, Hughes TE, Lekkas D, «Dental phenomics: advancing genotype to phenotype correlations in craniofacial research», in Aust Dent J, Australian Dental Association, 2014».
PMID:24611797
DOI:10.1111/adj.12156
- Thesleff I, «Current understanding of the process of tooth formation: transfer from the laboratory to the clinic», in Aust Dent J, 2013».
DOI:10.1111/adj.12102
- Peterkova R, Hovorakova M, Peterka M, Lesot H, «Three-dimensional analysis of the early development of the dentition», in Aust Dent J, Wiley Publishing Asia Pty Ltd on behalf of Australian Dental Association, 2014».
DOI:10.1111/adj.12130
- Lesot H, Hovorakova M, Peterka M, Peterkova R, «Three-dimensional analysis of molar development in the mouse from the cap to bell stage», in Aust Dent J, 2014».
DOI:10.1111/adj.12132
- Hughes TE, Townsend GC, Pinkerton SK, Bockmann MR, Seow WK, Brook AH, Richards LC, Mihailidis S, Ranjitkar S, Lekkas D, «The teeth and faces of twins: providing insights into dentofacial development and oral health for practising oral health professionals», in Aust Dent J, 2013».
DOI:10.1111/adj.12101
- Han J, Menicanin D, Gronthos S, Bartold PM, «Stem cells, tissue engineering and periodontal regeneration», in Aust Dent J, 2013».
DOI:10.1111/adj.12100
- Brook AH, Jernvall J, Smith RN, Hughes TE, Townsend GC, «The Dentition: The Outcomes of Morphogenesis Leading to Variations of Tooth Number, Size and Shape», in Aust Dent J, 2014».
DOI:10.1111/adj.12160
- Seow WK, «Developmental defects of enamel and dentine: challenges for basic science research and clinical management», in Aust Dent J, 2014».
PMID:24164394
DOI:10.1111/adj.12104
- Kieser JA, Farland MG, Jack H, Farella M, Wang Y, Rohrle O, «The role of oral soft tissues in swallowing function: what can tongue pressure tell us?», in Aust Dent J, 2013».
DOI:10.1111/adj.12103
- Slavkin HC, «Research on Craniofacial Genetics and Developmental Biology: Implications for the Future of Academic Dentistry», in J Dent Educ, 1983».
PMID:6573384
- Slavkin HC, «The Future of Research in Craniofacial Biology and What This Will Mean for Oral Health Professional Education and Clinical Practice», in Aust Dent J, 2014».
PMID:24433547
DOI:10.1111/adj.12105
- Littlewood SJ, Kandasamy S, Huang G, «Retention and relapse in clinical practice», in Aust Dent J, 2017».
DOI:10.1111/adj.12475
- Miamoto CB, Silva Marques L, Abreu LG, Paiva SM, «Impact of two early treatment protocols for anterior dental crossbite on children’s quality of life», in Dental Press J Orthod, 2018».
- Alachioti XS, Dimopoulou E, Vlasakidou A, Athanasiou AE, «Amelogenesis imperfecta and anterior open bite: Etiological, classification, clinical and management interrelationships», in J Orthod Sci, 2014».
DOI:10.4103/2278-0203.127547
- Mizrahi E, «A review of anterior open bite», in Br J Orthod, 1978».
PMID:284793
DOI:10.1179/bjo.5.1.21
- Pereira LM, Pinto AM, «Reductio ad Absurdum Argumentation in Normal Logic Programs», Arg NMR, 2007, Tempe, Arizona - Caparica, Portugal – in «Argumentation and Non-Monotonic Reasoning - An LPNMR Workshop».
- Castroflorio T, Talpone F, Deregibus A, Piancino MG, Bracco P, «Effects of a Functional Appliance on Masticatory Muscles of Young Adults Suffering From Muscle-Related Temporomandibular Disorder», in J Oral Rehabil, 2004».
PMID:15189308
DOI:10.1111/j.1365-2842.2004.01274.x
- Maeda N, Kodama N, Manda Y, Kawakami S, Oki K, Minagi S, «Characteristics of Grouped Discharge Waveforms Observed in Long-term Masseter Muscle Electromyographic Recording: A Preliminary Study», in Acta Med Okayama, 2019».
PMID:31439959
DOI:10.18926/AMO/56938
- Rudy TE, «Psychophysiological Assessment in Chronic Orofacial Pain», in Anesth Prog, 1990».
PMID:2085203 - PMCID:PMC2190318
- Woźniak K, Piątkowska D, Lipski M, Mehr K, «Surface electromyography in orthodontics - a literature review», in Med Sci Monit, 2013».
PMID:23722255 - PMCID:PMC3673808
DOI:10.12659/MSM.883927
- Liang X, Liu S, Qu X, Wang Z, Zheng J, Xie X, Ma G, Zhang Z, Ma X, «Evaluation of Trabecular Structure Changes in Osteoarthritis of the Temporomandibular Joint With Cone Beam Computed Tomography Imaging», in Oral Surg Oral Med Oral Pathol Oral Radiol, 2017».
PMID:28732700
DOI:10.1016/j.oooo.2017.05.514
- Solberg WK, Bibb CA, Nordström BB, Hansson TL, «Malocclusion Associated With Temporomandibular Joint Changes in Young Adults at Autopsy», in Am J Orthod, 1986».
PMID:3457531
DOI:10.1016/0002-9416(86)90055-2
- Kobs G, Didziulyte A, Kirlys R, Stacevicius M, «Reliability of ARCUSdigma (KaVo) in Diagnosing Temporomandibular Joint Pathology», in Stomatologija, 2007».
PMID:17637527
- Piancino MG, Roberi L, Frongia G, Reverdito M, Slavicek R, Bracco P, «Computerized axiography in TMD patients before and after therapy with 'function generating bites'», in J Oral Rehabil, 2008».
PMID:18197841
DOI:10.1111/j.1365-2842.2007.01815.x
- López-Cedrún J, Santana-Mora U, Pombo M, Pérez Del Palomar A, Alonso De la Peña V, Mora MJ, Santana U, «Jaw Biodynamic Data for 24 Patients With Chronic Unilateral Temporomandibular Disorder», in Sci Data, 2017».
PMID:29112190 - PMCID:PMC5674825
DOI:10.1038/sdata.2017.168
- Oliveira Mazzetto M, Almeida Rodrigues C, Valencise Magri L, Oliveira Melchior M, Paiva G, «Severity of TMD Related to Age, Sex and Electromyographic Analysis», in Braz Dent J, 2014».
DOI:10.1590/0103-6440201302310
- LeResche L, «Epidemiology of temporomandibular disorders: implications for the investigation of etiologic factors», in Crit Rev Oral Biol Med, 1997».
PMID:9260045
DOI:10.1177/10454411970080030401