3° Clinical case: Meningioma Abstract
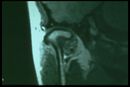
3° Clinical case: Meningioma
Article by: Gianni Frisardi· Flavio Frisardi
|
Abstract
This clinical case, referred to as Balancer, concerns a 60-year-old male patient who developed progressive postural and gait disturbances following repeated prosthetic rehabilitations aimed at correcting presumed occlusal instability. The case is analyzed using the same diagnostic framework previously applied to the clinical cases known as Mary Poppins and Bruxer, based on the distinction and weighting of dental and neurological contexts through a coherence demarcator ().
The clinical history initially suggested a functional postural disorder secondary to prosthetic imbalance and altered Centric Relationship. In line with a widespread assumption in dentistry, postural symptoms were attributed to occlusal disharmony and addressed through successive prosthetic remakes, including approaches guided by postural and pedanometric assessments. However, despite these interventions, the patient’s symptoms progressively worsened, raising doubts about the validity of an exclusively occlusal interpretation.
A critical issue highlighted by this case is the ambiguity of the term “correlation” when applied to Centric Relationship, occlusal stability, and posture. The chapter emphasizes the fundamental discrepancy between manually guided Centric Relationship—commonly used in orthognathic and prosthetic procedures—and the Neuro Evoked Centric Relationship obtained through transcranial stimulation of the trigeminal roots. The comparison between these two spatial mandibular positions reveals that a clinically acceptable occlusion may coexist with a profound neuromotor imbalance, undetectable by conventional dental criteria alone.
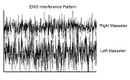
Electrophysiological assessment demonstrated that the apparent asymmetry observed in the interferential EMG pattern of the masseter muscles had limited diagnostic value when considered in isolation. When normalized to trigeminal Root-Motor Evoked Potentials, the EMG findings could be correctly interpreted, distinguishing functional variability from true asymmetry. More importantly, the neurological context revealed highly significant findings, including absence of the jaw jerk reflex and latency asymmetry of the masseter Silent Period, which cannot be explained by prosthetic or occlusal factors.
By applying the coherence demarcator, the diagnostic model assigns greater weight to the neurological assertions due to their intrinsic severity and pathophysiological relevance. Although minor dental abnormalities were present, their average diagnostic weight was low compared to the unequivocal positivity of the neurological findings. This logical weighting leads to a clear diagnostic prevalence of the neurological context, redefining the clinical interpretation of the patient’s postural disorder.
The Balancer case demonstrates that postural and gait disturbances attributed to occlusal imbalance may in fact represent early manifestations of structural neurological pathology. It also illustrates the risk of semantic shortcuts in clinical reasoning, particularly the uncritical use of terms such as “asymmetry” and “correlation” without adequate neurophysiological validation. The diagnostic framework presented aims to decrypt the machine language of the central nervous system and to prevent misdiagnosis by integrating dental and neurological data within a coherent, weighted model.
This case reinforces the need for caution when linking occlusion to posture and underscores the importance of electrophysiological testing in differentiating functional dental conditions from serious neurological disease.
🧠 Three guiding questions (with essential answers)
1️⃣ Is there a real scientific correlation between dental occlusion and body posture? – Current scientific evidence does not support a universal or direct causal relationship between dental occlusion and postural control. While some studies report associations, the results are highly variable and often lack clinical relevance. Any presumed correlation must therefore be evaluated case by case and validated with objective neurophysiological data.
2️⃣ Can Centric Relationship be considered a reliable reference for postural diagnosis? – Only if the concept of Centric Relationship is clearly defined. Manual or guided centric positioning may differ significantly from the Neuro Evoked Centric Relationship obtained through trigeminal root stimulation. Without distinguishing between these spatial references, correlations between occlusion, centricity, and posture become misleading and diagnostically unsafe.
3️⃣ Does electromyographic asymmetry necessarily indicate occlusal pathology? – No. Interferential EMG asymmetry is often a functional and unstable phenomenon. Its clinical significance can only be determined when normalized to organic reference signals such as trigeminal Root-Motor Evoked Potentials. Without this normalization, asymmetry may be incorrectly attributed to occlusal imbalance instead of underlying neurological dysfunction.
If you already have an approved account, click on your profile icon and return to the Book Index to read the complete chapter.
To access the full content, you must sign in via LinkedIn and request approval.
Bibliography & references
- Minervini G.; Franco R.; Marrapodi M.M.; Crimi S.; Badnjević A.; Cervino G.; Bianchi A.; Cicciù M., «Correlation between Temporomandibular Disorders (TMD) and Posture Evaluated through the DC/TMD: A Systematic Review with Meta-Analysis», 2023».
- An J.-S.; Jeon D.-M.; Jung W.-S.; Yang I.-H.; Lim W.H.; Ahn S.-J., «Influence of temporomandibular joint disc displacement on craniocervical posture and hyoid bone position», 2015».
- Abe S.; Kawano F.; Matsuka Y.; Masuda T.; Okawa T.; Tanaka E., «Relationship between Oral Parafunctional and Postural Habits and the Symptoms of Temporomandibular Disorders», 2022».
- Inchingolo A.D.; Pezzolla C.; Patano A.; Ceci S.; Ciocia A.M.; et al., «Experimental Analysis of the Use of Cranial Electromyography in Athletes and Clinical Implications», 2022».
- Perinetti G.; Türp J.C.; Primožič J.; Di Lenarda R.; Contardo L., «Associations between the Masticatory System and Muscle Activity of Other Body Districts», 2011».
- Julià-Sánchez S.; Álvarez-Herms J.; Cirer-Sastre R.; Corbi F.; Burtscher M., «The Influence of Dental Occlusion on Dynamic Balance and Muscular Tone», 2020».
- Heit T.; Derkson C.; Bierkos J.; Saqqur M., «The Effect of the Physiological Rest Position of the Mandible on Cerebral Blood Flow and Physical Balance», 2015».
- Bergamini M.; Pierleoni F.; Gizdulich A.; Bergamini C., «Dental Occlusion and Body Posture: A Surface EMG Study», 2008».
- Ishii T.; Narita N.; Endo H., «Evaluation of jaw and neck muscle activities while chewing using EMG transfer function analyses», 2016».
- Sharma T.; Veer K., «EMG classification using wavelet functions to determine muscle contraction», 2016».