System logic Abstract
Abstract: System Logic marks a shift in medical science when diagnosis must address living systems that are dynamic, layered, and only partially observable. This chapter explains why dentistry is being pushed toward System Logic by two converging pressures: the demand for objective clinical indices and the recognition that the logic of medical language is often inadequate for complex biological phenomena. Indices and constants, such as the Henderson–Hasselbalch equation for pH or laboratory-derived composite markers, provide measurable reference points for diagnosis and guidelines. Yet their validity is frequently debated because clinical reality is not exhausted by what a single index measures, and because interpretation, schools of thought, and hidden variables can distort what looks like “objective” data.
Orthodontics provides a concrete illustration. Outcome assessment traditionally relied on clinician experience and subjective judgment, then moved toward standardized indices such as the Peer Assessment Rating (PAR) and objective grading systems for casts and radiographs. These tools quantify deviation from alignment, compare pre- and post-treatment states, and support quality improvement. However, an index may be accurate for alignment without being sufficient to define “normocclusion”, which is a functional and systemic condition. Relapse can occur even with apparently good occlusal finishing, and long-term changes can undermine cutoff-based excellence, reminding clinicians that indices are models, not reality.
This tension connects directly to language logic. Classical logic forces bivalent conclusions (true/false), while probabilistic reasoning often becomes meaningful only inside narrow specialist contexts; both can oversimplify signals that are context-dependent, driven by feedback, and sometimes non-deterministic. The chapter therefore extends the previous motivation for fuzzy logic: instead of separating specialist know-how, System Logic encourages the superimposition of interdisciplinary contexts, so that complex clinical phenomena can be described with elastic but formal rules.
Systems Theory is presented as the formal backbone for System Logic. A system is modeled through inputs, states, and outputs across ordered time. In the masticatory domain, the trigeminal motor system is treated as a black box: controlled triggers (transcranial electrical stimulation) act as inputs, and measurable responses (latency and amplitude) define outputs. The chapter contrasts routine interferential EMG, whose reliability and diagnostic correlation with TMD, orofacial pain, and malocclusion remain contested, with evoked-potential methods that embody system behavior and expose higher-level dysfunction.
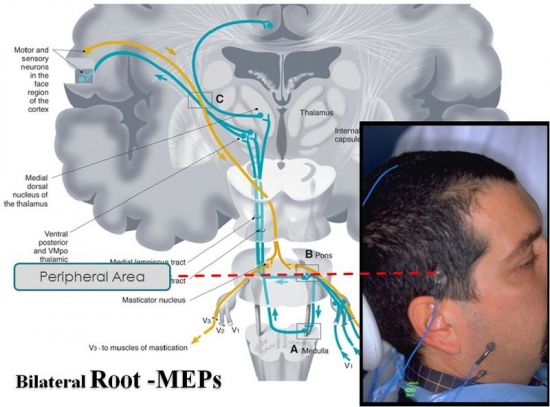
Clinically, this approach aims to reduce differential diagnostic error, avoid unnecessary dental interventions in patients whose orofacial symptoms arise from neurological disease, and enable earlier, life-saving detection by grounding indices in system behavior and repeatable measurements. A worked example is the Root-MEP protocol: a sequence of progressively greater stimuli delivered at ordered times produces multiple averaged traces in which latency decreases and amplitude increases as input rises. Because the response is evoked at the trigeminal motor root level, it captures system integrity at a higher hierarchical level than the occlusal observable. Repeating the protocol across epochs allows comparison of the same system over time, turning a qualitative clinical impression into reproducible variables, and preparing the reader for later chapters on diagnostic modeling in practice.
Three questions (Open Access)
(They provide measurable reference points, but they can miss hidden variables and functional system states; an index may quantify alignment without defining normocclusion or safety.)
(It moves beyond rigid true/false and narrow probabilistic framing by integrating elastic formal reasoning (including fuzzy concepts) with interdisciplinary context and feedback.)
(They treat the trigeminal motor system as a black box: a controlled input (trigger) produces measurable outputs (latency, amplitude) that track system integrity and can be compared across time.)
Access to full chapter
Full chapter available for Approved Members
Login to unlock the complete Book Index content.
<a class="pyr-link" href="/oauth/linkedin-login.php" style="display:inline-block; padding:10px 14px; border-radius:10px; text-decoration:none;">
✅ Login (Apply via LinkedIn)
</a>
- Xiao W, Yang Y, Shi J, Xu J, Zhu J, «The diagnostic efficacy and predictive value of combined lipoprotein laboratory indexes for atherosclerosis», in J Pak Med Assoc, 2020».
PMID:33177739 - Ferraro D, Bedin R, Natali P, Franciotta D, Smolik K, Santangelo M, Immovilli P, Camera V, Vitetta F, Gastaldi M, Trenti T, Meletti S, Sola P, «Kappa Index versus CSF Oligoclonal Bands in Predicting Multiple Sclerosis and Infectious/Inflammatory CNS Disorders», in Diagnostics (Basel), 2020».
PMID:33096861 - PMCID:PMC7589948
DOI:10.3390/diagnostics10100856
Template:OAref - Kayadibi H, Yilmaz B, Ozgur Yeniova A, Koseoglu H, Simsek Z, «Development and evaluation of a novel noninvasive index for predicting significant fibrosis, advanced fibrosis, and cirrhosis in patients with chronic hepatitis B infection», in Eur J Gastroenterol Hepatol., 2021».
PMID:33177385
DOI:10.1097/MEG.0000000000001973
- Sfondrini MF, Zampetti P, Luscher G, Gandini P, Gandía-Franco JL, Scribante A, «Orthodontic Treatment and Healthcare Goals: Evaluation of Multibrackets Treatment Results Using PAR Index (Peer Assessment Rating)», in Healthcare (Basel), 2020».
PMID:33182796 - PMCID:PMC7711869
DOI:10.3390/healthcare8040473
Template:OAref - Dyken RA, Sadowsky PL, Hurst D, «Orthodontic outcomes assessment using the peer assessment rating index», in Angle Orthod, 2001».
PMID:11407767
DOI:<0164:OOAUTP>2.0.CO;2 10.1043/0003-3219(2001)071<0164:OOAUTP>2.0.CO;2 - Richmond S, Shaw WC, O’Brien KD, Buchanan IB, Jones R, Stephens CD, Roberts CT, Andrews M, «The development of the PAR Index (Peer Assessment Rating): reliability and validity», in Eur J Orthod, Oxford University Press, 1992, Oxford UK».
PMID:1582457
DOI:10.1093/ejo/14.2.125 - Onyeaso CO, BeGole EA, «Associations between pretreatment age and treatment time with orthodontic treatment outcome: A comparison by means of two orthodontic indices», in Hell Orthod. Rev, MDPI, 2008, Basel, Switzerland».
Template:OAref - Hickman JH, «Directional edgewise orthodontic approach. 5», in J Clin Orthod, 1975».
PMID:1054697 - Firestone AR, Häsler RU, Ingervall B, «Treatment results in dental school orthodontic patients in 1983 and 1993», in Angle Orthod, 1997».
PMID:10022180
DOI:<0019:TRIDSO>2.3.CO;2 10.1043/0003-3219(1999)069<0019:TRIDSO>2.3.CO;2 - Cook DR, Harris EF, Vaden JL, «Comparison of university and private-practice orthodontic treatment outcomes with the American Board of Orthodontics objective grading system», in Am J Orthod Dentofacial Orthop».
PMID:15953896
DOI:10.1016/j.ajodo.2004.12.014 - Ramanathan C, «PAR index in the evaluation of the stability of the orthodontic treatment results. A review», in Acta Medica (Hradec Králové), 2006».
PMID:17438831
DOI:10.14712/18059694.2017.133 - Pangrazio-Kulbersh V, Kaczynski R, Shunock M, «Early treatment outcome assessed by the Peer Assessment Rating index», in Am J Orthod Dentofacial Orthop, 1999».
PMID:10229887
DOI:10.1016/s0889-5406(99)70277-5 - Templeton KM, Powell R, Moore MB, Williams AC, Sandy R, «Are the Peer Assessment Rating Index and the Index of Treatment Complexity, Outcome, and Need suitable measures for orthognathic outcomes?», in Eur J Orthod, 2006».
PMID:16648208
DOI:10.1093/ejo/cji120 - Angst C, Eliades T, Papageorgiou SN, «Stability of occlusal outcome during long-term retention: the time-dependent variation of the American Board of Orthodontics index», in Eur J Orthod, Zurich Open Repository and Archive, University of Zurich, 2021, Zurich, Switzerland».
PMID:32144422
DOI:10.1093/ejo/cjaa004 - Lyotard N, Hans M, Nelson S, Valiathan M, «Short-term postorthodontic changes in the absence of retention», in Angle Orthod, 2010».
PMID:20677953 - PMCID:PMC8929484
DOI:10.2319/010210-7.1
Template:OAref - Little RM, «Stability and relapse of dental arch alignment», in Br J Orthod., University of Washington, Seattle, 1990, Washington, USA».
PMID:2207055
DOI:10.1179/bjo.17.3.235 - Reitan K, Kvam E, «Comparative behavior of human and animal tissue during experimental tooth movement», in Angle Orthod, 1971».
PMID:4992550
DOI:<0001:CBOHAA>2.0.CO;2 10.1043/0003-3219(1971)041<0001:CBOHAA>2.0.CO;2 - Thilander B, «Dentoalveolar development in subjects with normal occlusion. A longitudinal study between the ages of 5 and 31 years», in Eur J Orthod, Oxford University Press on behalf of the European Orthodontic Society, 2009, Göteborg, Sweden».
PMID:19304760
DOI:10.1093/ejo/cjn124 - Behrents RG, Harris EF, Vaden JL, Williams RA, Kemp DH, «Relapse of orthodontic treatment results: growth as an etiologic factor», in J Charles H. Tweed Int Found, 1989».
PMID:2634695 - Lang G, Alfter G, Göz G, Lang GH, «Retention and stability--taking various treatment parameters into account», in J Orofac Orthop, 2002».
PMID:11974450
DOI:10.1007/s00056-002-0036-2 - Steinnes J, Johnsen G, Kerosuo H, «Stability of orthodontic treatment outcome in relation to retention status: An 8-year follow-up», in Am J Orthod Dentofacial Orthop, 2017».
PMID:28554448
DOI:10.1016/j.ajodo.2016.10.032 - de Freitas KM, Janson G, de Freitas MR, Pinzan A, Henriques JF, Pinzan-Vercelino CR, «Influence of the quality of the finished occlusion on postretention occlusal relapse», in Am J Orthod Dentofacial Orthop, 2007».
PMID:17920494
DOI:10.1016/j.ajodo.2007.02.051 - Hoybjerg AJ, Currier GF, Kadioglu O, «Evaluation of 3 retention protocols using the American Board of Orthodontics cast and radiograph evaluation», in Am J Orthod Dentofacial Orthop, 2013».
PMID:23810041
DOI:10.1016/j.ajodo.2013.02.022 - Nett BC, Huang GJ, «Long-term posttreatment changes measured by the American Board of Orthodontics objective grading system», in Am J Orthod Dentofacial Orthop, Elsevier Inc, 2005».
PMID:15821689
DOI:10.1016/j.ajodo.2004.03.029 - Casko JS, Vaden JL, Kokich VG, Damone J, James RD, Cangialosi TJ, Riolo ML, «Objective grading system for dental casts and panoramic radiographs», in Am J Orthod Dentofacial Orthop, 1998».
PMID:9810056
DOI:10.1016/s0889-5406(98)70179-9 - von Bertalanffy L, «General System Theory: Foundations, Development, Applications», George Braziller, 1968, New York».
ISBN: 978-0807604533
DOI:10.1001/archpsyc.1969.01740200123021 - Template:Cita web
- Template:Cita web
- Reaz MB, Hussain MS, Mohd-Yasin F, «Techniques of EMG signal analysis: detection, processing, classification and applications (Correction)», in Biol Proced Online, 2006».
PMID:16799694 - PMCID:PMC1455479
DOI:10.1251/bpo115 - Masci C, Ciarrocchi I, Spadaro A, Necozione S, Marci MC, Monaco A, «Does orthodontic treatment provide a real functional improvement? A case control study», in BMC Oral Health, BioMed Central Ltd, 2013».
PMID:24152806 - PMCID:PMC3827987
DOI:10.1186/1472-6831-13-57
Template:OAref - Moazzam AA, Habibian M, «Patients appearing to dental professionals with orofacial pain arising from intracranial tumors: a literature review», in Oral Surg Oral Med Oral Pathol Oral Radiol, 2012».
PMID:23036798
DOI:10.1016/j.oooo.2012.06.017 - Merton PA, Morton HB, «Stimulation of the cerebral cortex in the intact human subject», in Nature, 1980».
PMID:7374773
DOI:10.1038/285227a0 - Cruccu G, Berardelli A, Inghilleri M, Manfredi M, «Functional organization of the trigeminal motor system in man. A neurophysiological study», in Brain, 1989».
PMID:2804615
DOI:10.1093/brain/112.5.1333
- Haebeom L, Hyunho K, Jungkuk K, Hwan-Sup O, Young-Jae P, Young-Bae P, «Feasibility study of transfer function model on electrocardiogram change caused by acupuncture», in BMC Complement Altern Med, 2017».
PMID:28178964 - PMCID:PMC5299648
DOI:10.1186/s12906-017-1615-5
Template:OAref - Smith RJ, Kamali G, Hays M, Coogan C, Crone NE, Kang JY, Sarma SV, «Transfer Function Models for the Localization of Seizure Onset Zone From Cortico-Cortical Evoked Potentials», in Front Neurol, Frontiers in Neurology, 2020».
PMID:33362689 - PMCID:PMC7758451
DOI:10.3389/fneur.2020.579961
Template:OAref
