Introduction Abstract: differenze tra le versioni
Nessun oggetto della modifica |
Nessun oggetto della modifica |
||
| Riga 1: | Riga 1: | ||
__NOTITLE__ | |||
{{main menu it | {{main menu it | ||
|link to German= Hauptseite | |link to German= Hauptseite | ||
| Riga 13: | Riga 14: | ||
== Abstract == | == Abstract == | ||
The masticatory system — including teeth, occlusion, muscles, temporomandibular joints, and central and peripheral neural control networks — cannot be adequately described as a simple biomechanical mechanism. Rather, it must be interpreted as a '''complex adaptive system''', in which function emerges from non-linear interactions among morphological, neuromuscular, and neurophysiological components. Within this framework, many clinical manifestations that appear “abnormal” according to traditional models do not represent errors or therapeutic failures, but instead constitute genuine '''signals of paradigmatic crisis''', in the sense originally described by Thomas Kuhn. | |||
The classical approach to the diagnosis and treatment of masticatory disorders has historically been based on predominantly morphological categories, particularly the concept of “malocclusion.” However, clinical experience and increasing experimental evidence demonstrate that occlusal form, when considered in isolation, is not a reliable predictor of function. Patients with marked occlusal discrepancies may exhibit stable neuromuscular balance, whereas individuals with morphologically “correct” occlusions may develop pain, instability, and functional relapse. For this reason, Masticationpedia proposes a conceptual shift from “malocclusions” to “'''occlusal dysmorphisms'''”, emphasizing the distinction between morphological description and functional meaning. | |||
Electrophysiological tests — including mandibular reflexes, motor evoked potentials, and the mechanical silent period — represent fundamental tools for investigating the functional level of the masticatory system. They allow objective assessment of neuromuscular symmetry, reflex control, and the integration between peripheral structures and the central nervous system. The evidence presented shows that '''functional symmetry''' can be preserved even in the presence of pronounced occlusal dysmorphisms, through adaptive neuroplastic mechanisms that stabilize the system over time. | |||
This perspective has decisive clinical implications. Masticatory rehabilitation — whether orthodontic, prosthetic, or surgical — can no longer be oriented exclusively toward achieving static occlusal stability. Instead, it must aim for '''dynamic functional stability''', verifiable through reproducible neurophysiological parameters. The absence of such integration represents one of the main causes of therapeutic failure and late relapse, often erroneously attributed to poor patient compliance. | |||
Within this framework, the OrthoNeuroGnathodontic model emerges as an integrated diagnostic-therapeutic strategy combining morphological evaluation, functional analysis, and clinical electrophysiology. This model does not merely correct form, but recognizes the central role of the nervous system in maintaining masticatory equilibrium. The adoption of measurable functional criteria thus makes it possible to overcome a reductionist approach and to align clinical practice with the principles of complex systems medicine, paving the way for more stable, predictive, and scientifically grounded treatments. | |||
<gallery mode=" | <gallery mode="slideshow" widths="100"> | ||
File:Occlusal Centric view in open and cross bite patient.jpg|''' | File:Occlusal Centric view in open and cross bite patient.jpg|'''Figure 1a:''' Centric occlusal view of a patient with crossbite and open bite. | ||
File:Bilateral Electric Transcranial Stimulation.jpg|''' | File:Bilateral Electric Transcranial Stimulation.jpg|'''Figure 1b:''' Bilateral transcranial electrical stimulation: masseter muscle symmetry. | ||
File:Jaw Jerk .jpg|''' | File:Jaw Jerk .jpg|'''Figure 1c:''' Jaw jerk reflex: confirmed functional symmetry. | ||
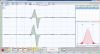
File:Mechanic Silent Period.jpg|''' | File:Mechanic Silent Period.jpg|'''Figure 1d:''' Mechanical silent period: balanced bilateral activation. | ||
</gallery> | </gallery> | ||
=== | === Three guiding questions (with essential answers) === | ||
;1) | ;1) What: in what sense is the masticatory system a complex system (and not merely biomechanical)? | ||
It is a system in which morphology (teeth/occlusion) and neurophysiological control (trigeminal system and central/peripheral networks) interact non-linearly: function emerges from the integration of components, not from isolated form. | |||
;2) | ;2) Why: why is “malocclusion” often an insufficient category from a functional and diagnostic standpoint? | ||
Because “malocclusion” primarily describes a morphological asymmetry, which may not correspond to dysfunction: neuromuscular adaptations can preserve symmetry and functional performance even in the presence of evident discrepancies. | |||
;3) | ;3) How: how do electrophysiological tests change diagnosis and therapeutic strategy (from form to function)? | ||
They introduce measurable criteria of symmetry and neuromuscular control (reflexes, evoked potentials, silent period), enabling function-based diagnosis and guiding therapies aimed at functional stability and relapse prevention. | |||
---- | ---- | ||
<div style="border:1px solid #d8d8d8; border-radius:14px; padding:18px 20px; background:#fafafa; margin:22px 0;"> | <div style="border:1px solid #d8d8d8; border-radius:14px; padding:18px 20px; background:#fafafa; margin:22px 0;"> | ||
<span style="font-size:20px;">🔒 <b> | <span style="font-size:20px;">🔒 <b>Would you like to read the full chapter?</b></span><br> | ||
<span style="font-size:18px; line-height:1.45;"> | <span style="font-size:18px; line-height:1.45;"> | ||
If you already have an approved account, sign in with LinkedIn and return to the Book Index: the link will take you to the complete version of the chapter. | |||
</span> | </span> | ||
</div> | </div> | ||
| Riga 87: | Riga 88: | ||
* Avivi-Arber L; Martin R; Lee JC; Sessle BJ. The Face Sensorimotor Cortex and its Neuroplasticity in Health and Disease. ''J Dent Res''. 2019;98(11):1184–1194. doi:10.1177/0022034519865385 | * Avivi-Arber L; Martin R; Lee JC; Sessle BJ. The Face Sensorimotor Cortex and its Neuroplasticity in Health and Disease. ''J Dent Res''. 2019;98(11):1184–1194. doi:10.1177/0022034519865385 | ||
* Iwata K; Sessle BJ. Neural Basis of Orofacial Functions in | * Iwata K; Sessle BJ. Neural Basis of Orofacial Functions in Healt* | ||
* | |||
Versione delle 14:19, 29 dic 2025
__NOTITLE__
Introduction Abstract
Article by: Gianni Frisardi
|
Abstract
The masticatory system — including teeth, occlusion, muscles, temporomandibular joints, and central and peripheral neural control networks — cannot be adequately described as a simple biomechanical mechanism. Rather, it must be interpreted as a complex adaptive system, in which function emerges from non-linear interactions among morphological, neuromuscular, and neurophysiological components. Within this framework, many clinical manifestations that appear “abnormal” according to traditional models do not represent errors or therapeutic failures, but instead constitute genuine signals of paradigmatic crisis, in the sense originally described by Thomas Kuhn.
The classical approach to the diagnosis and treatment of masticatory disorders has historically been based on predominantly morphological categories, particularly the concept of “malocclusion.” However, clinical experience and increasing experimental evidence demonstrate that occlusal form, when considered in isolation, is not a reliable predictor of function. Patients with marked occlusal discrepancies may exhibit stable neuromuscular balance, whereas individuals with morphologically “correct” occlusions may develop pain, instability, and functional relapse. For this reason, Masticationpedia proposes a conceptual shift from “malocclusions” to “occlusal dysmorphisms”, emphasizing the distinction between morphological description and functional meaning.
Electrophysiological tests — including mandibular reflexes, motor evoked potentials, and the mechanical silent period — represent fundamental tools for investigating the functional level of the masticatory system. They allow objective assessment of neuromuscular symmetry, reflex control, and the integration between peripheral structures and the central nervous system. The evidence presented shows that functional symmetry can be preserved even in the presence of pronounced occlusal dysmorphisms, through adaptive neuroplastic mechanisms that stabilize the system over time.
This perspective has decisive clinical implications. Masticatory rehabilitation — whether orthodontic, prosthetic, or surgical — can no longer be oriented exclusively toward achieving static occlusal stability. Instead, it must aim for dynamic functional stability, verifiable through reproducible neurophysiological parameters. The absence of such integration represents one of the main causes of therapeutic failure and late relapse, often erroneously attributed to poor patient compliance.
Within this framework, the OrthoNeuroGnathodontic model emerges as an integrated diagnostic-therapeutic strategy combining morphological evaluation, functional analysis, and clinical electrophysiology. This model does not merely correct form, but recognizes the central role of the nervous system in maintaining masticatory equilibrium. The adoption of measurable functional criteria thus makes it possible to overcome a reductionist approach and to align clinical practice with the principles of complex systems medicine, paving the way for more stable, predictive, and scientifically grounded treatments.
Three guiding questions (with essential answers)
- 1) What
- in what sense is the masticatory system a complex system (and not merely biomechanical)?
It is a system in which morphology (teeth/occlusion) and neurophysiological control (trigeminal system and central/peripheral networks) interact non-linearly: function emerges from the integration of components, not from isolated form.
- 2) Why
- why is “malocclusion” often an insufficient category from a functional and diagnostic standpoint?
Because “malocclusion” primarily describes a morphological asymmetry, which may not correspond to dysfunction: neuromuscular adaptations can preserve symmetry and functional performance even in the presence of evident discrepancies.
- 3) How
- how do electrophysiological tests change diagnosis and therapeutic strategy (from form to function)?
They introduce measurable criteria of symmetry and neuromuscular control (reflexes, evoked potentials, silent period), enabling function-based diagnosis and guiding therapies aimed at functional stability and relapse prevention.
🔒 Would you like to read the full chapter?
If you already have an approved account, sign in with LinkedIn and return to the Book Index: the link will take you to the complete version of the chapter.
- Heft MW, Fox CH, Duncan RP, «Assessing the Translation of Research and Innovation into Dental Practice», in JDR Clin Trans Res, 2019».
DOI:10.1177/2380084419879391
- «Exposure Science in the 21st Century. A Vision and a Strategy», National Research Council, Division on Earth and Life Studies, 2012».
ISBN: 0-309-26468-5
- Liu L, Li Y, «The unexpected side effects and safety of therapeutic monoclonal antibodies», in Drugs Today, 2014, Barcellona».
DOI:10.1358/dot.2014.50.1.2076506
- James Frederick Ferrier. Institutes of Metaphysic. 1854. (Internet Encyclopedia of Philosophy: Ferrier).
- Srivastava S. «Verifiability is a core principle of science», in Behav Brain Sci, Cambridge University Press, 2018».
DOI:10.1017/S0140525X18000869
- Evans M. «Measuring statistical evidence using relative belief», in Comput Struct Biotechnol J, 2016».
DOI:10.1016/j.csbj.2015.12.001
- Amrhein V; Greenland S; McShane B. «Scientists rise up against statistical significance», in Nature, 2019».
DOI:10.1038/d41586-019-00857-9
- Rodgers JL. «The epistemology of mathematical and statistical modeling: a quiet methodological revolution», in Am Psychol, 2010».
DOI:10.1037/a0018326
- Meehl P. The problem is epistemology, not statistics: replace significance tests by confidence intervals and quantify accuracy of risky numerical predictions. 1997.
- Sprenger J; Hartmann S. «Bayesian Philosophy of Science. Variations on a Theme by the Reverend Thomas Bayes», Oxford University Press, 2019».
- Wasserstein RL; Schirm AL; Lazar NA. «Moving to a World Beyond p < 0.05», in Am Stat, 2019».
DOI:10.1080/00031305.2019.1583913
- Boon M; Van Baalen S. «Epistemology for interdisciplinary research – shifting philosophical paradigms of science», in Eur J Philos Sci, 2019».
DOI:10.1007/s13194-018-0242-4
- Boon M. «An engineering paradigm in the biomedical sciences: Knowledge as epistemic tool», in Prog Biophys Mol Biol, 2017».
DOI:10.1016/j.pbiomolbio.2017.04.001
- Guven Y. «Scientific basis of dentistry», in J Istanb Univ Fac Den, 2017».
DOI:10.17096/jiufd.04646
- Smaglyuk LV; Voronkova HV; Karasiunok AY; Liakhovska AV; Solovei KO. «Interdisciplinary approach to diagnostics of malocclusions (review)», in Wiad Lek, 2019».
- Avivi-Arber L; Lee JC; Sessle BJ. Motor cortex neuroplasticity associated with dental occlusion. J Dent Res. 2015;94(12):1751–1759. doi:10.1177/0022034515596345
- Avivi-Arber L; Martin R; Lee JC; Sessle BJ. The Face Sensorimotor Cortex and its Neuroplasticity in Health and Disease. J Dent Res. 2019;98(11):1184–1194. doi:10.1177/0022034519865385
- Iwata K; Sessle BJ. Neural Basis of Orofacial Functions in Healt*